The COVID-19 pandemic has not only led to a devastating loss of lives but also exacerbated the socioeconomic inequalities of our world. While wealthier nations have been able to cushion their economies from lockdowns by infusing trillions of dollars, poorer economies have witnessed large-scale destruction of livelihoods. According to the WHO, millions of individuals are expected to fall back into poverty and improvements in health outcomes could be set back by years. In such a scenario, the importance of developing innovative models to facilitate universal health coverage and achieve SDG 3 (Good Health and Wellbeing) becomes even more imperative. This blog highlights how SonoCare, a Nigerian social enterprise, leverages technology to deliver health services to bottom-of-the-pyramid (BOP) beneficiaries while operating a sustainable business model.
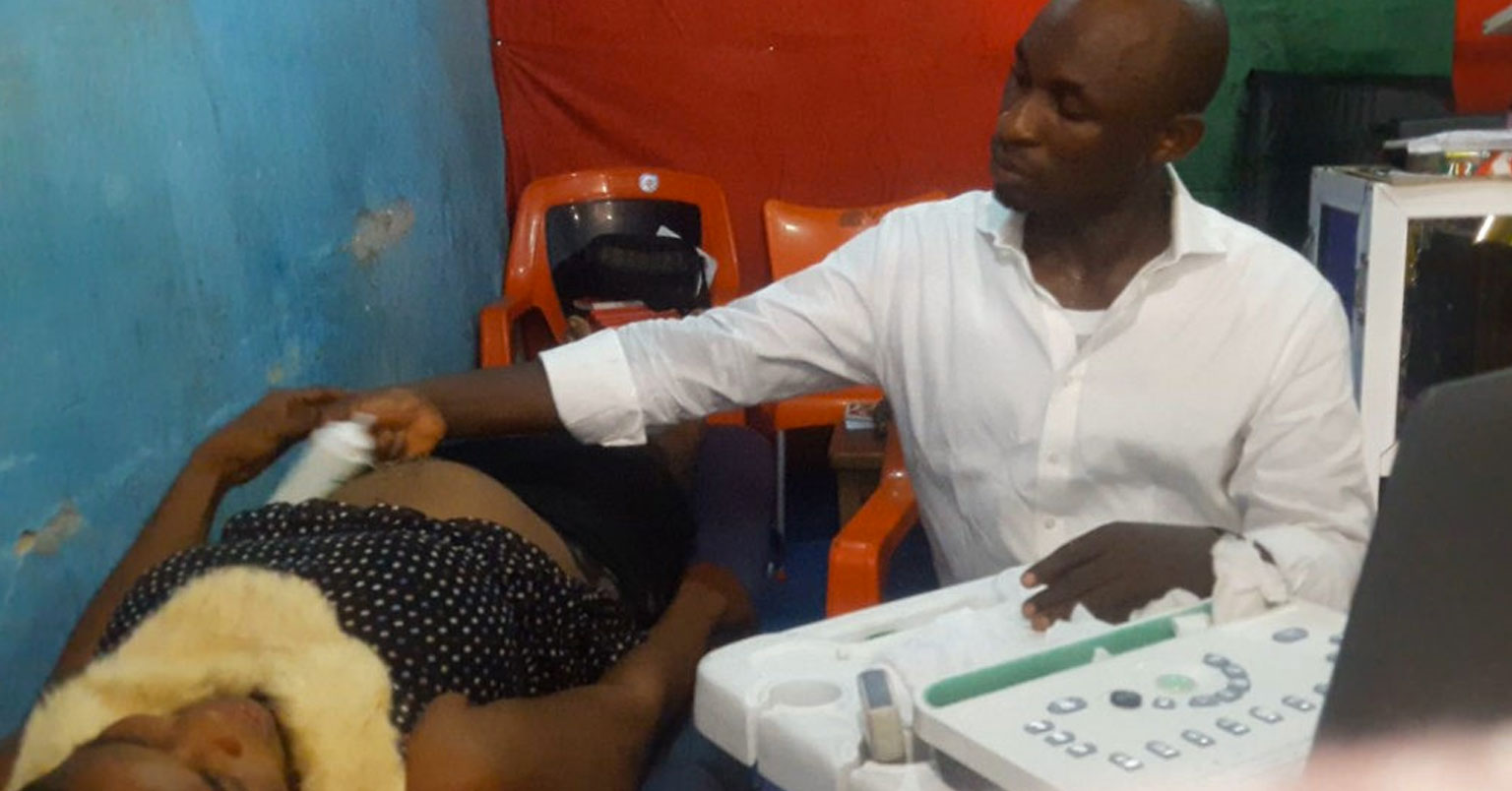
Dr Moses Enokela founded SonoCare in 2015 after he witnessed how the lack of ultrasound examinations in Nigeria was leading to preventable maternal mortality. His solution to the dilemma was to bring the examinations to pregnant women rather than have them seek out the service. SonoCare does this by integrating the diagnostic equipment with vehicles and thereby providing medical imaging at point-of-care. The ‘mobile ultrasound labs’ that SonoCare operates help overcome two key challenges healthcare providers face: improving access to services and reducing costs to patients. The mobility of the equipment allows the social enterprise to provide services to last-mile rural mothers who have the greatest need in terms of improving access to quality healthcare. Furthermore, the lack of up-front capital required to set up decentralised mobile labs compared to physical clinics means that SonoCare can charge a lower price for its services than other providers. The dual benefits of accessibility and low costs incentivises women to get ultrasounds, which reduces the likelihood of complications during pregnancy.
My interactions with Dr Moses go back to 2018 when I worked with Gray Matters Capital (GMC) in Atlanta, USA, fresh out of college. This was my first exposure to the world of social innovation. Dr Moses’ passion for improving the lives of his patients using limited resources led to GMC investing $150,000 into SonoCare. The funds were utilised to scale operations by developing a digital application to facilitate communication with customers and deploying more mobile units to cater to 200,000+ pregnancies by 2020. Today, SonoCare has evolved into a leader in Nigeria’s health-tech and telehealth space and has seen large-scale adoption due to the COVID-19 pandemic. It offers a comprehensive digital platform with a suite of various services from E-Prescriptions to Rapid Ambulance Response. The start-up has also set up its own physical clinics to meet growing demand and has partnered with several hospitals to train ultrasound technicians.
SonoCare, to me, represents the promise of social innovation in fostering digitally-enabled health solutions. As the importance of technology becomes central to the delivery of essential services, there needs to be a global effort to build an ecosystem that advances health equity through innovation. I believe that social enterprises such as SonoCare should be considered key stakeholders in future policies and roadmaps on digital health as they have the potential to play an outsized role in improving health outcomes. Furthermore, to catalyse ‘digital health inclusion’, governments, and multilateral agencies need to focus on: i) strengthening the ICT infrastructure in the Global South to make digital services more accessible to BOP populations; and ii) incubating social enterprises that can leverage the ICT infrastructure to deliver innovative health interventions to underserved communities. Additionally, because such enterprises strive to operate for-profit business models that are not dependant on a constant flow of grants, they can help drive more risk-averse commercial capital (such as venture capital) towards closing the $2.5 trillion annual SDG financing gap, which has so far primarily been financed by a limited pool of public and philanthropic funds. It’s time we look beyond the traditional top-down approach to deliver healthcare and embrace innovative localised solutions that can be scaled for global impact.
Associate at Impact Investors Council (IIC)
-
This author does not have any more posts.